Electrochemotherapy (ECT) for STS journey -same day & day 1 post op
So, after being diagnosed with a 2nd kind of cancer in addition to OSA and amputation of front R-Leg, In April of 2015 I had a mass removed from my back Left Leg. I was offered these options. definite radiation, pallative radation, or metronomic chemotherapy. After much research and consultation, I determined, pallative had too much risk of site damage in the long run, only because my girl was still doing well and no other signs of cancer were in her body (at least not visible or growing). Definite radiation, was recomended by 1 oncologist and not recommended by 2 others for various reasons, mostly due to her other OSA and the feeling their call was based on her OSA could flare up (its been 19months, common let be a bit positive) and the other one was because he was concerned if she did get localized burning it would be irritating on an already 3 legged dog. plus going under sedation or anesthesia every day for 18 days. Sooo my research began, of course I want to do natural approach as well, but In my heart I wanted to be sure to kill the remaining cells. So we began IV chemo AGAIN, since she tolerated it so well the first time, no side effects.
I came upon this procedure ECT, electrochemotherapy, teh procedure is based on injection chemo either IV or into the tumor, or in her case the scar from removal, or both depending what is needed. Yesterday we drove over 6hrs to the closest place that offered it. It is a newer procedure in the states but seems to be used all over Australia as well as Europe the UK …etc. I researched to the best of my ability as the studies are not all long term and consistent, but what I did see looked really promising and made logical sense.
After the chemo is injected, (in my girls case in 2 ways, IV and incisional, to cover all the potential left over cells) they wait about 5mn or a bit more depending, and then use various electrodes and “zap” the area the mass is in or was in (stimulating) this allows the cancer cell membrane to open up and uptake of the chemo into the cells, thus killing the cells. (in a nut shell) her whole procedure took about 15mn (varies depending on how many sites and other variables) Sedation or anesthesia.(short) Mine was a bit longer as she had a tiny “lipoma” by her eye and I wanted it bx too but when she started she decided to remove it, which was great, even a lipoma, it was so close to the eye, you hate to have problems with it later on. so yay! shes still sending it out but she said it acted like all the lipomas shes seen.
So my experience is below, considering, my girl was very fatigued from the trip as she decided to balance on her one front leg between the seats for 6 hrs.. uug.. i was tired for her, we came the night before, thank goodness.
-Post procedure:, she seemed kinda tender sore, not to touch but mostly walking had a bit of a hard time, if she had 4 legs would probably favor it some. However, I have to take into consideration Neka’s history, she has a TPLO on the same leg and though they said the hardware would not interfer, I wonder a bit if the electric current traveled up the leg as its a pretty big jolt. She was more tender in her knee than teh actually site when walking, like when I pushed on her knee, she kind of buckled out. She has a bit of redness and swelling.. totally expected as they zap it and inject it… Ugg hated seeing her like that, but it also made me realize that if I did nothing and it were to grow back, how debilitating it could be, so something short lived for longer pain free life!!?? Plus she was fatigued prior from the trip and not wanting to rest in car, so multiple contributing factors!!??
Day after procedure–shes still pretty sore meaning tender to walk on, especially because of her 3 legs and her already orthopedic issues.. Again, TPLO on the same leg and suspect tear on the other, so shes moving a bit funny, again, tender in the knee, not the actuall site. I figure its gotta be like a car accident, your muscles and bones get jolted, where someone with no issues recovers quick, but someone whos got prior problems would feel it a bit more. Plus all that I read with reactions, never stated anything about that, if anything they stated no initial reaction or side effects. So I have to take into account her prior ortho issuses. But personality and demeanor is the all good. Just tired from the trip.
THe plan of care is with her to have 2 treatments 1 week apart, because I also plan on doing metronomic to just cover my basis, and I did 3 rounds of prior IV chemo. I will see how she does over this next week to determine if continuing is justified. Its a super cool procedure and outcomes seem sooo promising with minimal to no side effects, very short procedure. It can be repeated even if it starts to grow back, or if I change my mind I can also do radiation. Oh, another thing is, all my pictures helped the new oncologist get an idea of what was removed prior and how she recovered, interestingly she mentioned because she had an odd swelling reaction after the surgery, that maybe some blood vessels got cut off which could cause maybe a more sever reaction with definite radiation. So, food for thought guys, document everything, it could always help for later procedures.
Started with a STS: neg aspirate (dog gone aspirates)

1-8-15_ I had been questioning this mass for almost a year, had it aspirated 2 months before this pic, which came back as only fatty cells, this pic represents, when I felt like it was growing and changing but was told it was the same. That sit hard in my gut, and I payed for it 3 months later.
Surgical removal 4-6-15

4-8-15_2days post op, pathology stated clean lateral margins, but deep margins were dirty. My surgeon was awesome. Grade 3 STS.. ugg
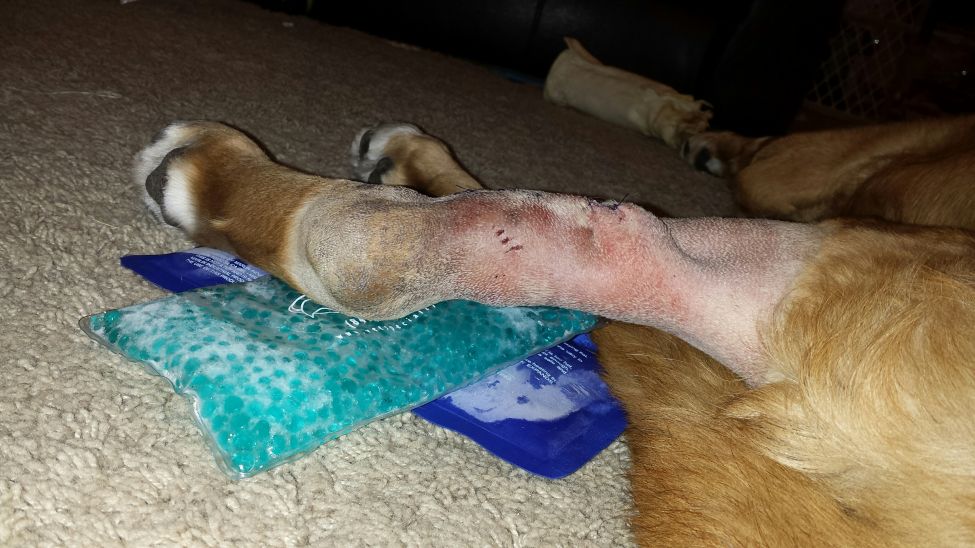
4-9-15_ 3 days post op……uh oh, wierd swelling reaction, no fever, just odd reaction. Always check with your vet if you see this. She was ok, but could have been something bad.
ECT procedure pics below: 7-29-15


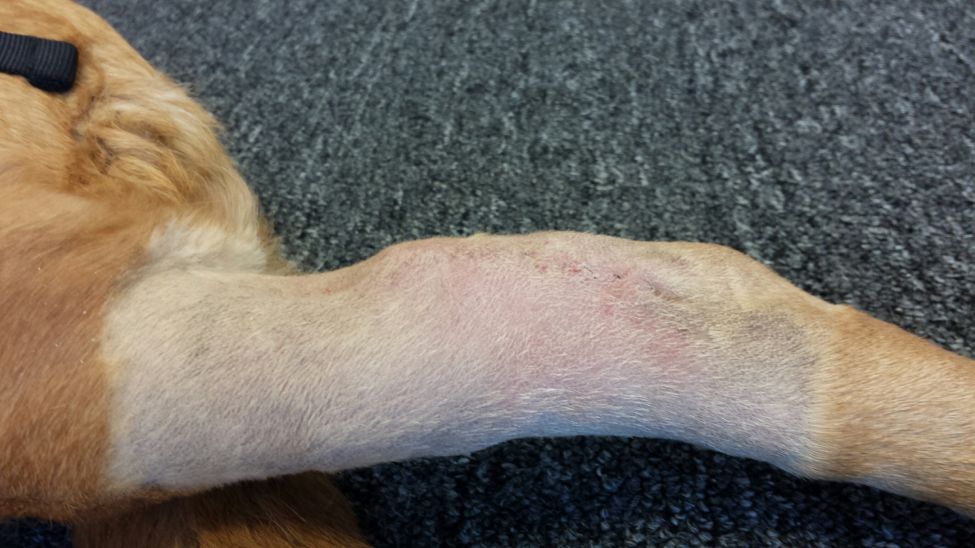
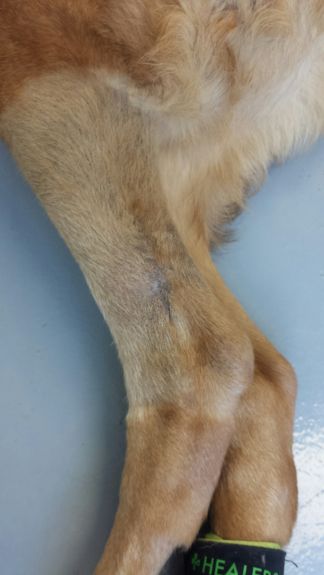
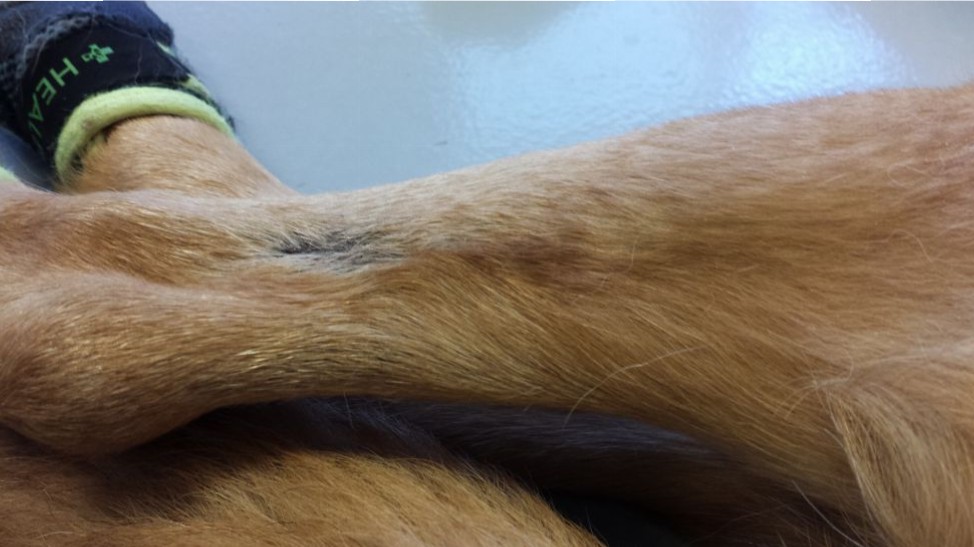
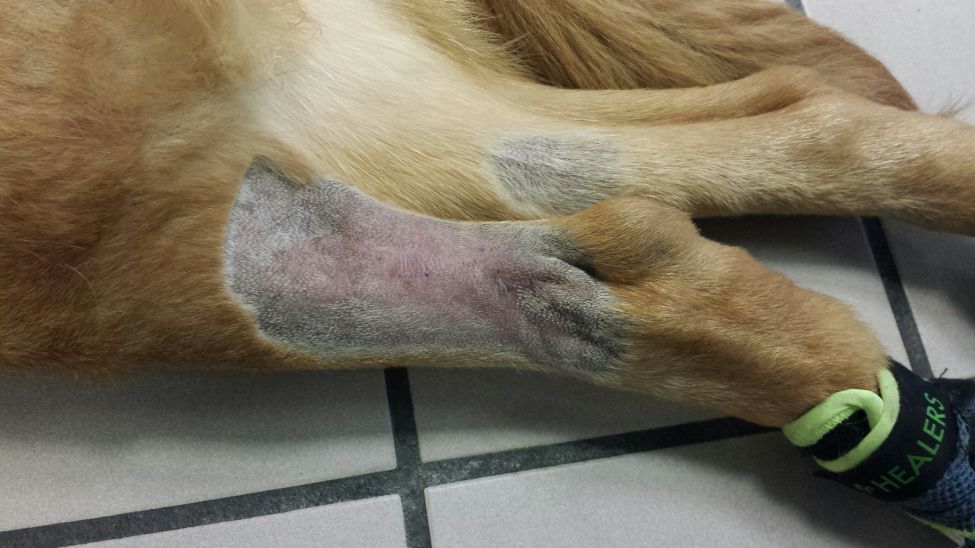
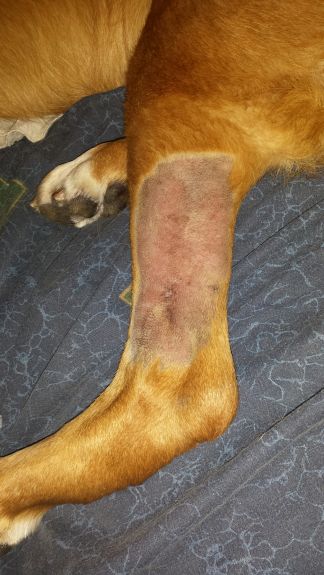
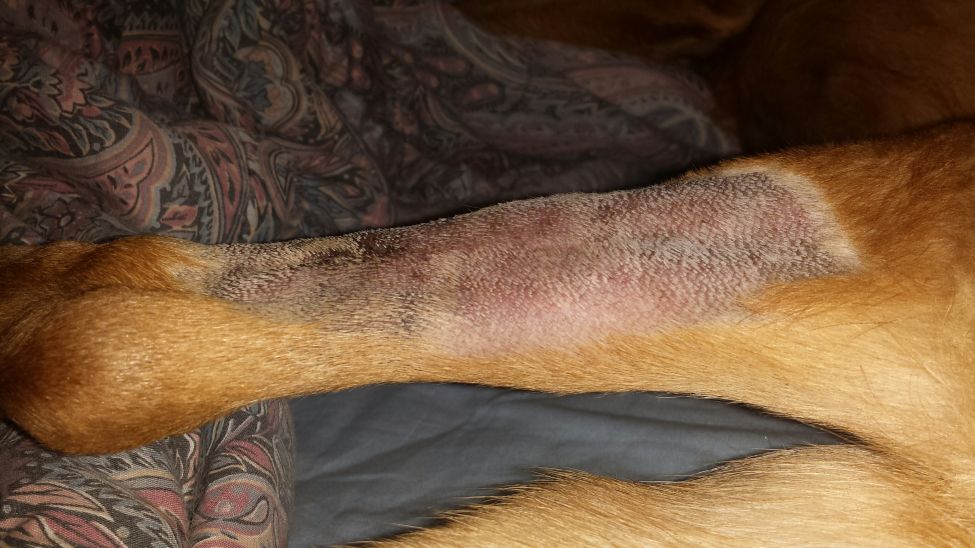
July 30th, 2015 at 1:26 am
WOW!! WOW ON SO MANY LEVELS!!!
You absolutely astound me with the amount of research you have done and the vast knowledge you have just now shared! Neka’s blog is INVALUABLE! You have done a magnificent job m of chronicling everything about her journey so far.
I can’t wait for Jerry to see this! She LOVES having all sorts of new and exciting options to share with others!
Thank you sooooooo much for taking the time the document this amazing journey you and your precious Neka are taking together. Talk about an inspiration and a treatment that offers hope…WOW!
Ice cream and cake for Neka after every treatment…and in between! She deserves it!
With love and appreciation,
Sally and Alumni Happy Hannah and Merry Myrtle too!
July 30th, 2015 at 1:39 am
Thank you, Your very kind..
It wasnt my plan, but with the procedure being so new and hopefully more studies will pop up. This site inspired me to offer some more documented subjects to hopefully give someone else an easier job of that 1 more option you wish you knew about.
Though, remembering her rx may be different because of added knee issues and some muscle atrophy. Im sure all contribute.
The Vet student assigned to her case, made a comment about, Your moms trying to make you live forever. I said.. no, Im just doing my part, for as long as all her insides and brain is working the same, then Im doing my part, the rest is up to her.
If theres an option with minimal side effects, especially systemically, and cost is about the same as a chemo session, why not!! IF no harm can come, its worth a shot.
July 30th, 2015 at 10:43 am
Really like your responsem to the vet tech! Well said…good philosophy!!
Just curious…was the original lump on her leg hard or more of a “fluid” feel to the touch? Did it “move” under the skin?
Thanks for any additional insight you can share. You and Neka are such a valuable source for great information that may, indeed, transform lives…starting with sweet Neka!!!
xoxoxoxoxox
August 1st, 2015 at 11:21 pm
sorry for delay. Well the feel was tricky.. so It was present for more than a year, and at that time is was more flat and moveable, but as it grew because there was limited skin and area to move it got tighter if that makes sense, When her leg was relaxed (not standing on it) I could almost lift it somewhat and could feel an attachment point. but when standing the skin tightened becoming less movable. The feel was not hard but not squishy, and as it grew it got firmer, to me is was “rubbery” The thing that upset me the most is 6 months prior and I stated I felt like it was growing as when I was palpating it, to me I felt like it was changing. But since aspirate was negative, it was dismissed. Even though I know what I felt and still asked about it, Im pretty sure my onco thought I was crazy, I even consulted with the surgeon who also said it was probably ok, then when I came back in april and said this thing is too big and grew and could potentially cause issue, they were both like, Oh yes thats a concern, we need to remove it..(not to have anger in my voice, its just, if we missed it, its one thing, but because I kept asking about it and was actually a proactive owner, I think they either thought she wouldnt live that long or I was crazy, pretty sure its one of those 2 things) I learned a hard-hard lesson, I think In my future if shes ever under and theres a mass easily removable Id just have them do it. Even if it was a negative biopsy, it was still growing in an area that could have been an issue.
though I was really, really, really upset, mostly because I was asking about it. But because If i was a bit more aggressive maybe we would have had a better chance of getting clean margins. It was mentioned that it could have started benign and changed over time since it was there for so long. Hence, early persistence.
July 30th, 2015 at 11:20 am
SO SO pawesome! Really glad to hear it went well and she’s rockin. Heck I’d feel pretty beat up too if I got poked like that. She seems to be recovering like a champ though.
OH my gosh this is really exciting for all of you, and this community too. We’re all learning from your ECT experience which by all accounts seems to be going great. I also want to say that I totally admire your upbeat, steady-as-she-goes, stay strong attitude. The way you’re taking into account her previous ortho history when thinking about how she’s recovering today, well that show’s a steady, rational, calm attitude that is so needed when undergoing something like this. You ROCK just like Neka!
Thank you soooo much for sharing your journey, we ow you a debt of gratitude. Give Neka a smooch from us and keep us posted OK?
July 30th, 2015 at 7:41 pm
Thank you so much for sharing about this procedure. Always glad to hear of new ways to treat this crappy disease one day soon there maybe a cure or at least I hope so.
Keep us posted on her recovery & the procedures.
xooxxo
Michelle & Angel Sassy
July 4th, 2017 at 9:08 am
Hello,
I’m looking into the possibility of electrochemotherapy being an option for my Reggies STS which was surgically removed but needing to do additional treatments because we were not able to get clean margins. I’m curious to know how things are going now for Neka?
July 4th, 2017 at 1:39 pm
Hello,
I highly recommend this procedure as an option to treat STS. Unfortunately my girl past away 1 Yr ago from a 3rd cancer of hemangiosarcoma of the heart and liver, however I was able to keep her STS of her leg at bay with no return up until her passing. she had it surgically removed then I was able to do 2 regular IV chemo treatments after surgery (I couldn’t do more regular infusions because we had used a lot of chemo sessions for her OSA), then I took her in and had the ETC, its so minimally evasive, outpatient, and so quick of a treatment,I did so much research prior to proceeding with the treatment, including calling multiple doctors that performed the procedure, there were very few studies for such a high grade STS which is what my girl had, so I knew the results may not be the same as a lower grade, however, with a properly developed protocol she really exceeded in recovery and healing. So really almost 10months-1 full year from surgical removal of a high grade or grade 3 STS and no return.
where are you located?
what grade STS does he have? location on body?
Let me know if you have any more questions, Im pretty medically versed.
July 7th, 2017 at 6:26 pm
Thank you for getting back to me so quickly. I’m very sorry to hear your girl passed. It sounds like she was so lucky to have a mom like you looking out for her. His specific tumor is a low grade nerve sheath SLS. It was located right below his front right elbow. The surgeon felt pretty confident he got everything but the lab results showed dirty margins. He referred me to VCA Animal Diagnostics of Dallas onocology. The doctor presented me with several options one being a 6 treatment of chemotherapy that is injected directly into the scar/tumor area (5-fu). The other option was 18 sessions of radiation and then the electrochemotherapy treatment. Or just wait and see. My impression from the Dr. Was he seemed to favor the radiation because the succes rate. He indicated that the electrochemotherapy success percentage was somewhere in the middle of radiation and the (5-fu). But what does that all really mean? I’m noticing they are considering cancer free to mean no cancer for 2 years. So basically my understanding is Reggie probably won’t die from this particular cancer but what I’m trying to do is safe his leg. He’s very active and becomes depressed when he can’t play. He’s very sensitive and hates being in the car and driving and has extreme anxiety when going to the vet. I just can’t imagine putting him through 18 sessions of radiation. I do want to do what’s best but i also don’t want to go overboard making his life a living hell when there are other good options available